
Section 3:
Role of Physical Therapy in Your Post-Op Recovery
Learn about the 6 Key Roles that Pelvic Floor Physical Therapy plays in your recovery:
Pre-Surgical Preparation
Immediate Post-Surgical Preparation
Long Term Care Recovery and Rehabilitation
Preventing Recurrence
Enhancing your Quality of Life
Ongoing Support and Monitoring

Pre-Surgical Preparation:
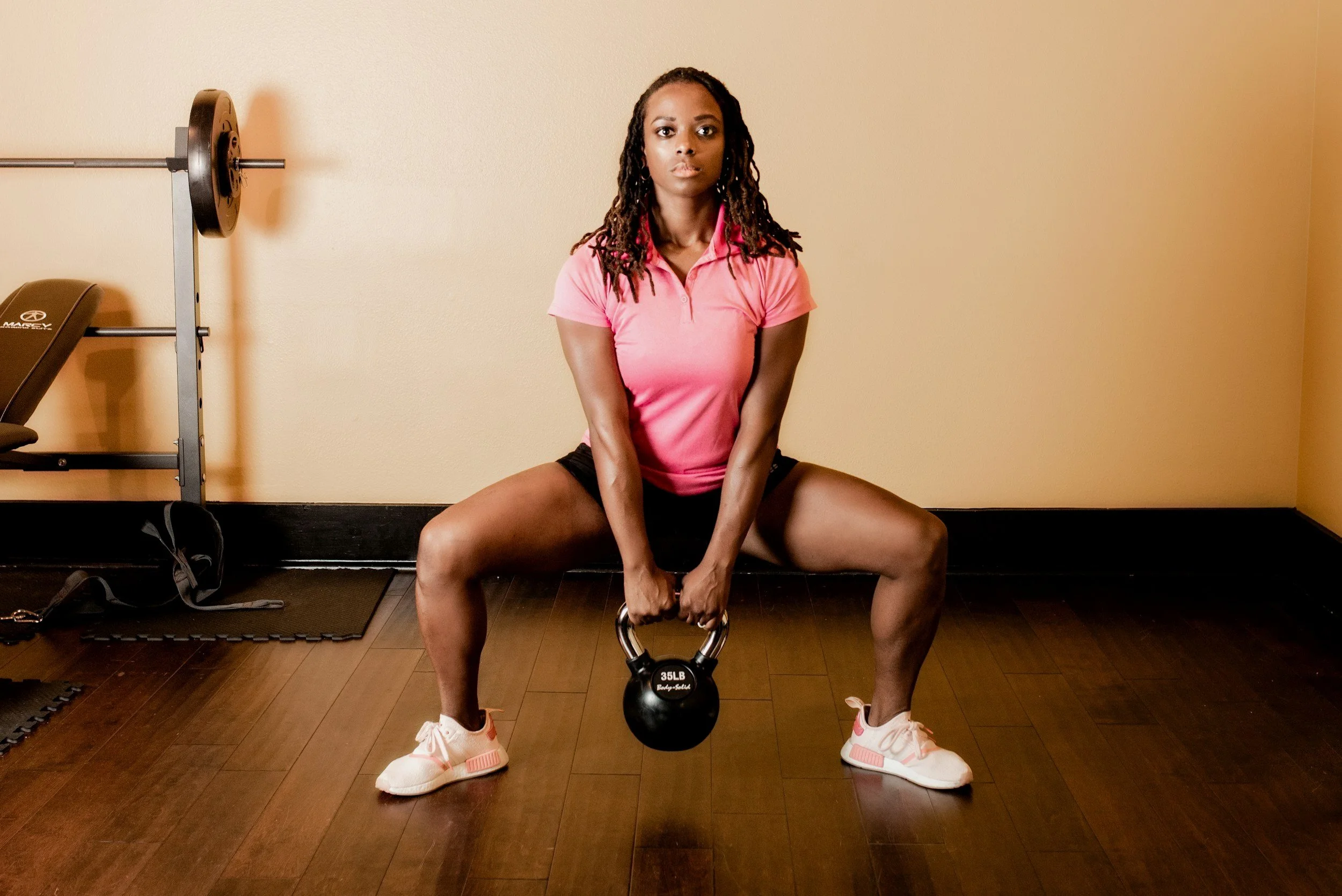
Implement a Pelvic Floor Strengthening Program: This program may include specific exercises and techniques to target the pelvic floor muscles such as kegels, as well as the surrounding supporting muscles, such as the core, glutes, and hip muscles.
Beware of your Body Mechanics: Identify when you are feeling your symptoms. Have you found strategies to help minimize these?
Manage your Bowels: Drink water, start a walking program, perform a bowel massage, use over the counter medication and reduce your stress. The bowel system loves a routine, implement one prior to surgery.
Optimize your fitness program: Find what you enjoy doing (i.e stretching, walking, swimming, pilates, etc), Start moving!
Immediate Post-Op Preparation:
Pain Management: Medications, rest, and gentle movements are introduced to reduce discomfort and promote healing.
Activity Limitations: A reduction in heavy lifting, straining, and excessive movement is crucial in this recovery stage. Understanding your body's limitations is key to preventing complications.
Positioning & Movement: Post-surgical instructions include how to safely transition between sitting, standing, and lying down to protect the surgical site. Gentle walking is often encouraged to avoid stiffness and promote circulation.
This site will provide a weekly guide and exercise to help with your immediate post surgical recovery.

Long Term Care Recovery and Rehabilitation:

The long-term recovery phase typically lasts around 8 to 12 weeks after surgery, marking the period when returning to normal activities often begins. During this time, you will receive guidelines on safely reintroducing functional movements, performing appropriate exercises, and gradually resuming daily activities. Toward the end of the recovery phase, pelvic floor rehabilitation with a specialized physical therapist may be included to help you achieve your goals and build confidence.
Prevent Reoccurance:
Preventing reoccurrence after prolapse surgery involves a combination of lifestyle adjustments, physical therapy and improved attention to your pelvic floor. Integrating different strategies into your daily life can help reduce your chance of reoccurrence and maintain long term pelvic health. This can start prior to your surgery and continue into post surgery. Key strategies include:
Pelvic Floor Exercises
Optimal Lifting and Body Mechanics
Weight Management
Avoiding Constipation and Straining
Improving Posture with Exercises
Gradually Returning Back to Activities
Maintain a Healthy Lifestyle (i.e: no smoking and staying active)



Enhance Quality of Life:

Physical therapy can significantly enhance quality of life after prolapse surgery by addressing both physical and emotional aspects of recovery. Here are several ways pelvic floor physical therapy can help:
Restoring muscle function and improving muscle coordination
Improve pelvic floor relaxation and reduce pain or discomfort
Build up strength to support posture and abdominal stability
Personalize exercise programs and provide strategies to improve on body mechanics
Improve bowel and bladder function
Reduce scar restriction and improve blood flow
Empower your ability to return back to activity
Provide techniques to improve confidence.
Ongoing Support and Monitoring:
By learning proper body mechanics, core stability, and pelvic floor exercises, you can prevent further pelvic issues and maintain a healthy pelvic floor for years to come. Ongoing physical therapy can help you maintain strength and flexibility, preventing future prolapse or related complications.
Physical therapy provides individualized attention, adapting exercises and techniques to suit your unique recovery needs. Whether you need to focus on strengthening, relaxation, mobility, or functional movement, a therapist can create a plan that supports your goals and maximizes recovery.
